One aim the president and Democratic 2020 challengers share is the desire to bring down the price of prescription drugs. But is that already happening, or are prices still climbing? The two parties disagree, and it depends on how they’re measuring drug prices.
President Donald Trump has claimed, “Last year, for the first time in over 50 years, drug prices went down,” while Sen. Kamala Harris says on her website that pharmaceutical companies “increased drug prices by 10.5 percent over the past six months alone.”
The president is referring to a measure of what consumers and insurers pay at retail pharmacies (though it hasn’t been 50 years since that index dropped), and Harris is referring to list prices for a basket of drugs, according to their campaigns.
The problem with drug prices is that they can be measured in different ways, and there’s not one comprehensive measure of all prices, or alternatively, of what people, insurers and the government ultimately pay. There are rebates and discounts and behind-the-scenes negotiations, as well as common retail drugs, specialty drugs and physician-administered medications. The introduction of generics and how prescribing patterns change also impact what is spent.
“There is no measure that actually does what we’re talking about,” Joseph Antos, a health policy expert at the American Enterprise Institute, told us. There’s “no good measure of drug pricing trends.”
Richard Evans, founder and general manager of SSR Health, an investment research firm, told us the answer to whether prices have gone up or down depends on which drugs we’re talking about and at which point in the supply chain. “List prices are rising for brands, but the net prices are falling,” he said, with “net” meaning after rebates, discounts, coupons and fees are deducted.
SSR Health’s analysis captures 90% of brand sales and measures price-per-unit trends. In inflation-adjusted terms, list prices have gone up by 3.3% in the first quarter of this year, while net prices declined by 4.1%, the company found.
The Trump administration is relying on the consumer price index for prescription drugs, a measure of drug price inflation that aims to capture what consumers, along with their insurance companies or other payers, are paying for a basket of retail prescriptions. The Bureau of Labor Statistics’ most recent figures show the CPI for prescriptions dropped by 2% from June 2018 to June 2019.
The CPI has its shortcomings. Experts point out that it doesn’t include specialty drugs, which tend to be expensive, and its ability to accurately measure what insurers pay is hindered by what pharmacies can report. But Barry Bosworth a senior fellow at the Brookings Institution, told us the CPI for prescription drugs is “the best that is available.”
That doesn’t mean that Democrats don’t have support for some of their claims, but their measures of drug prices have limitations, too, usually pertaining to a subset of drugs, only brand-name drugs or only drug list prices that have increased.
The list price affects consumers’ copays, coinsurance or deductibles. Evans said insurance beneficiaries at the prescription counter are “experiencing the list price inflation,” because their out-of-pocket amounts are based on the list prices.
But the net price paid for a drug can vary considerably from its list price. Evans said the average difference between list and net for brand-name drugs is 47%, as of the end of the first quarter of the year.
We’ll take a closer look at these measures and what politicians have claimed.
The CPI
Over the past several months, Trump has repeatedly made some version of the claim, “Drug prices are coming down, first time in 51 years because of my administration.” Last week, in a July 17 campaign rally in North Carolina, he said it again, claiming drug prices went down “for the first time in over 50 years.” Five days later, on July 22, he upped that to “53 years.”
Trump’s campaign pointed to the CPI when we inquired about the president’s claim. But it hasn’t been that long since the year-over-year change in the CPI for drugs dipped below zero. Before the recent decline, the CPI had dropped in July 2013, from the year prior.
The president has used the December 2017 to December 2018 decline of 0.6% as the first “calendar year” drop since December 1971 to December 1972, which is 46 years prior, not 50. But looking at each month’s 12-month change, which fluctuates, the December decrease was the first in about five-and-half years.
However, the CPI now has decreased year-over-year in six of the past seven months, a string of declines that hasn’t occurred since the early 1970s.
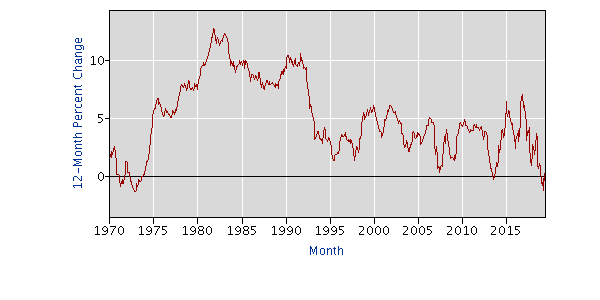
Here’s a look at the 12-month change in the CPI for prescription drugs since BLS began tracking this measure:
The measure showed a 2% decrease in June, the largest on record, as Alex Azar, secretary of the Department of Health and Human Services, noted on July 16 in a cabinet meeting.
“So, new data in for June that shows that, again, prescription drug prices are going down,” Azar said. “The Department of Labor’s inflation measure for prescription drug prices, it continues to go down. … The biggest decrease in over 50 years.” (It’s technically 49 years.)
The CPI for prescription drugs, as BLS explains, “measures price change of drugs purchased with a prescription at a retail, mail order, or internet pharmacy.” The price in this case is “the total reimbursement to the retailer from the patient and all eligible payers for a single prescription.” That means it includes payments to the pharmacy from consumers, insurance companies or other payers, such as Medicare Part D.
Like other inflation indexes, the measure is based on a sample. It’s a sample of retail pharmacies, and the drug prices measured are a sample drawn from the last 20 prescriptions dispensed at each pharmacy. It makes adjustments for the introduction of generics six months after brand-name drugs’ patents expire.
It’s a broad measure of transactions at retail pharmacies, but that means it doesn’t measure everything.
Walid Gellad, director of the Center for Pharmaceutical Policy and Prescribing at the University of Pittsburgh, told us that to answer whether drug prices have gone up or down “really depends on what drug prices you’re talking about.” The CPI, he pointed out, excludes some types of high-price drugs.
“Is it important that the CPI shows drug prices went down? Yes,” he said in an email. “But it’s misleading to rely solely on the CPI, because it excludes physician and hospital administered drugs, and does not sample specialty pharmacies. … It also doesn’t adequately account for new drugs that enter the market at [a] very high price.”
Gellad mentioned the 2018 Express Scripts Drug Trend Report, which found that spending for traditional drugs went down by 5.8% from 2017 to 2018, while spending on specialty drugs went up 9.4%. Express Scripts, a pharmacy benefit management company, said that those specialty drugs “account for 44.7 percent of total drug spending, up 3.9 percent from 2017.”
“To clear it up for your readers, some drugs went up, some went down!” Gellad said.
The CPI also doesn’t capture rebates that drug manufacturers pay to pharmacy benefit managers or insurers, of course, since those payments occur outside of the retail transaction. Rebates are used as incentives by the manufacturers to get their drugs on insurers’ formularies, or in a preferred placement on those formularies. (For more on rebates, see this explainer video from the Kaiser Family Foundation.)
Antos said it’s difficult to precisely measure what insurers are paying.
BLS is “trying to do the impossible,” Antos told us in a phone interview, “which is isolate the amount that is paid in total on behalf of consumers plus by consumers directly for a drug that they buy at the pharmacy. And as you know, there’s enough complication in the way drug pricing is set, the way formularies are determined,” including rebates and other fees, “that muddy the water.”
A 2018 report published by the Brookings Institution and National Bureau of Economic Research said the CPI relies “disproportionately” on cash transactions, which only make up about 7% of the retail drug market, because pharmacies are limited in sharing information from electronic transactions from third-party payers. And it raised questions about how well the CPI was able to capture the transitions to generic medications.
Despite the concerns about the CPI’s limitations, when we contacted the lead author of that report, Brookings’ Bosworth, he said the Trump administration is “right to rely on the CPI,” calling it “the best that is available.”
Bosworth wrote in an email to FactCheck.org that there’s “enormous variability in drug price changes and there is no means of incorporating the initial cost of new drugs” in the CPI. “Still the methods used to calculate the CPI average are superior to the alternatives,” he said, noting that it’s a broad index “that makes a major effort to be representative of all retail sales of prescription drugs” and factors in the introduction of generics.
But does the CPI tell us that drug prices have declined? Bosworth said he would “accept [the recent change] as indicative of a sustained change.”
Evans, of SSR Health, said, “It is factually correct to say drug prices are coming down,” provided that the speaker means “drug prices at the point of sale.” He added that it’s possible consumers have seen price growth or a decline; there’s no index that calculates only what the consumer pays out of pocket.
Similarly, Antos said politicians should stick more closely to the technically correct statement — that the CPI prescription drug price component went down. But what the president and other politicians tend to say “is something that’s looser and therefore has an element of correctness to it but can be misleading.”
Our fact-checking colleagues at the Washington Post and PolitiFact also have looked into these claims, finding concerns from experts over what the CPI can show and that there’s no one, perfect measure on drug prices.
What Other Measures Say
Democratic presidential candidates, meanwhile, have pointed to other reports, but those, too, have their limitations.
For instance, Harris, in her plan to lower drug prices, said that “families have been slapped with double-digit price increases on 2,500 drugs since Trump took office.”
Sen. Amy Klobuchar also used the 2,500 figure in the first Democratic debate.
“The president literally went on TV, on Fox, and said that people’s heads would spin when they see how much he would bring down pharmaceutical prices. … Instead, 2,500 drugs have gone up in double-digits since he came into office,” Klobuchar said. That refers to a list of drug prices from Pharmacy Benefit Consultants, promoted in a tweet in March 2018 by Andy Slavitt, a former acting administrator for the Centers for Medicare and Medicaid Services.
But those figures are from more than a year ago and the claims refer only to those drugs, not drug prices overall.
Last month, CNBC found there had been nearly 1,600 — not 2,500 — drug price increases of 10% or more since Trump took office, according to Michael Rea, founder of Rx Savings Solutions. Rea’s figure came from public disclosures of price increases.
Harris also says in her plan that pharmaceutical companies “increased drug prices by 10.5 percent over the past six months alone,” referring to a Politico story on other figures from Rx Savings Solutions that the company confirmed to FactCheck.org.
“In the first six months of the year, prices for 3,443 medicines rose, compared to 2,919 last year — yet the overall size of the price hikes was lower than in the previous period — 10.5 percent compared to 15 percent,” Politico reported.
Note that the 10.5% increase refers to those 3,443 drugs — not drug prices overall.
The Harris campaign argues that these measures of list prices, before rebates or other discounts are applied, are the more relevant measures. The CPI, a campaign spokesperson, told us “doesn’t reflect what consumers are actually paying overall because it doesn’t take rebates into account,” and the index is “representative of popular drugs, making it less likely to include newer or less-prescribed drugs, which are more expensive.”
As we said, the list prices, before rebates, do matter to consumers because their out-of-pocket copays and coinsurance amounts are based on the list prices.
SSR Health has found that the increase in brand-name list prices has slowed. List prices went up 3.3% in real terms in the first quarter of this year but 6.3% in the first quarter of 2018. The company said this was due to a decrease in the number of price hikes of more than 10%, and it said political pressure, dating back to a 2015 tweet about drug pricing from then-presidential candidate Hillary Clinton, had had an impact.
The Harris campaign pointed to another measure showing thousands of brand-name drug price hikes. An Associated Press analysis found 2,712 price increases among branded drugs in early January, with a median increase of 5%. Those numbers are down from 3,327 increases in January 2018, with a median hike of nearly 9%, the AP reported, based on data from Elsevier, a health data firm.
Sen. Kirsten Gillibrand’s campaign also pointed the Washington Post Fact Checker to such analyses after she claimed in a CNN interview this month that Trump “promised to lower prescription drug prices and failed.”
The Bureau of Labor Statistics also provides a producer price index, which measures the price drug manufacturers receive. Richard G. Frank, a professor of health economics at Harvard Medical School, told the Washington Post that he tends to look at that measure, “because it is closer to what manufacturers are selling drugs for.” It has been flat in recent months but hasn’t shown year-over-year declines like the CPI. Pointing to that and other market measures, Frank said, “I think the evidence points to slowed growth not negative growth.”
Trump’s Policies
Trump has claimed that drug prices are coming down “because of my administration,” but experts questioned that.
While Trump has focused on lowering drug prices, Antos told us any administration’s policies wouldn’t have had an impact on the CPI this soon. “It is fair to say that three years into a presidential administration” — meaning any administration, he said — “one should not jump to the conclusion that anything they may have done would have been the primary reason for that particular result.”
It would take a while, more than three years, to have an impact in either direction — causing prices to go up or down, he said.
Evans gave one reason for the drop in the CPI, but it didn’t have anything to do with the Trump administration’s policies: a decrease in markups by retail pharmacies. He said there are more pharmacies than needed in the country, so the pharmacy benefit managers have leverage in their negotiations with retail outlets, causing pharmacies to lower their markup amounts.
Express Scripts credits its “clinical innovations” for a decrease in actual drug costs paid by its insurance plans from 2017 to 2018 while list prices went up.
A Trump campaign spokesperson pointed to the administration’s efforts to more quickly approve generic drugs. Generic applications faced a backlog during the Obama administration, which began to take steps to expedite the approval process, as a 2017 Brookings Institution paper explains. The Food and Drug Administration has continued to prioritize generics.
PricewaterhouseCoopers noted that generic approvals have been “steadily on the rise” since fiscal year 2014. In fiscal 2018, 781 generics were approved, up significantly from the 409 approved in 2014.
But it’s unclear how much of an impact this would have had on overall drug prices. Antos said the increase in the introduction of generics “would’ve had an impact but it wouldn’t have had a huge impact,” and Evans said he didn’t think the decline in the CPI could be explained by a shift to generics, as there weren’t any “big blockbuster” generic approvals.
In 2016, the percentage of prescriptions filled with generics was already at 89% (but just 27% of total drug costs), according to a study from the QuintilesIMS Institute, conducted for the Generic Pharmaceutical Association. Update, Aug. 1: In 2018, generics made up 90% of prescriptions filled and 22% of total drug spending, according to the Association for Accessible Medicines (formerly the Generic Pharmaceutical Association), citing IQVIA data.
The Trump campaign also pointed to some drug companies announcing price freezes in 2018 in response to Trump revealing a plan to lower drug prices (though some companies then planned to raise them in 2019). Other actions by the Trump administration either haven’t been implemented for long or haven’t yet gone into effect, while others don’t pertain to retail drugs measured by the CPI or have been blocked by the courts. For instance, the Trump administration issued a new policy for Medicare Advantage plans, allowing them to use “step therapy,” which requires enrollees to use lower-cost alternatives to more expensive physician-administered drugs for new prescriptions. But the policy didn’t take effect until Jan. 1, and experts told us last year it was unclear how much impact the policy could have on spending or price.
The administration has pushed price transparency policies, but a court recently blocked its proposed rule to force drug companies to list prices in TV ads for pharmaceuticals.
Democratic proposals include setting caps on drug prices based on what other countries pay (Harris), punishing companies for unjustified price hikes and importing drugs from Canada (Gillibrand), and ending pay-for-delay deals that keep generics off the market and allowing the government to negotiate Medicare Part D prices (Klobuchar).
In touting their plans, politicians have their pick of statistics on drug prices. We’d caution voters to question what exactly those statistics are measuring.

 FactCheck.org Rating:
FactCheck.org Rating: 
 FactCheck.org Rating:
FactCheck.org Rating: 